January 2020
Juvenile Cellulitis in a Four-Month-Old Chinese Crested Puppy
Journey of Four-Month-Old Chinese Crested Puppy “Sadie”: A Case of Severe Juvenile Cellulitis
By Drs. Amanda Brown and Charan Ganta
CASE SUMMARY
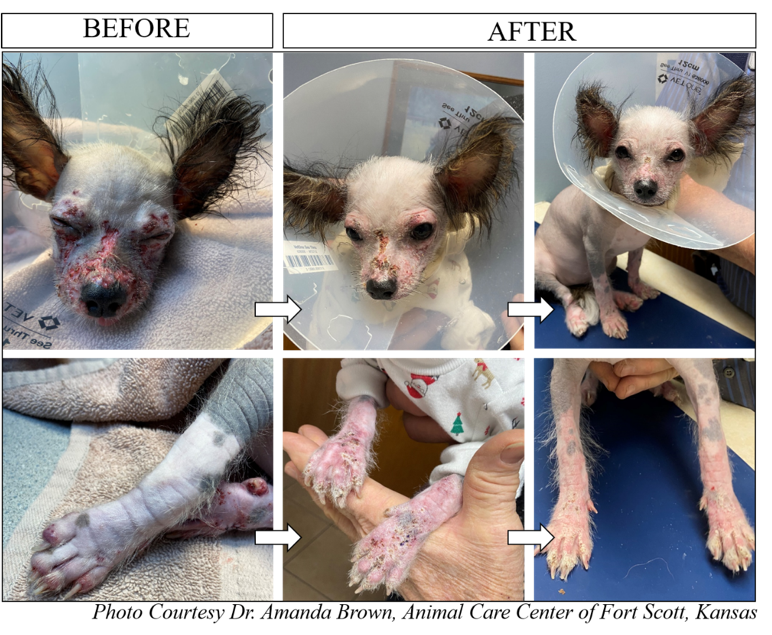
A four-month-old Chinese Crested puppy named Sadie was presented with a history of swollen eyes with reddening blisters and ulcers (Figure: BEFORE). Juvenile cellulitis was suspected based on the age and lesion distribution. She was immediately started on prednisolone at 1mg/kg q12h and clindamycin 7.5mg/kg body weight q12h and sent home with an E-collar. After 5 days, the skin lesions seemed to have improved. After 2 days, the owner reported that Sadie was not sleeping well. Prednisolone was decreased to 0.5mg/kg and butorphanol was prescribed. After two days, the lesion was severe with blisters that ruptured to form ulcers on the face and feet.
Multiple skin punch biopsies were collected and submitted to KSVDL for additional diagnostics. Histopathological examination of the skin biopsies showed marked pyogranulomatous dermatitis, furunculosis with ulceration and mild pyoderma.
|
|
Based on the clinical presentation, distribution of the lesions, age and initial response to prednisone therapy, canine juvenile cellulitis was diagnosed. Prednisolone was increased to 1mg/kg, q12h clavamox was initiated at 7.5mg/kg q12h. Clindamycin was discontinued. In addition, Science Diet D/D Duck® and potato formula along with benadryl at night were initiated. After 2 days on the increased level of prednisone, the lesion began to heal. The scabs began to dry up and Sadie became more comfortable. By the seventh day, the lesions on the face were completely resolved. A maintenance dose of prednisolone and clavamox were prescribed. After two weeks Sadie showed complete recovery (AFTER). No visible enlargement of lymph nodes or joints was noticed during the course of the disease.
CANINE JUVENILE CELLULITIS
Canine juvenile cellulitis, also known as “puppy strangles,” is an uncommon skin disease in puppies (also diagnosed rarely in adult dogs) that manifests as bilaterally symmetrical pyogranulomatous dermatitis of the face, favoring the periocular skin, pinnae, lips, muzzle, and occasionally the limbs, abdomen, thorax, vulva, prepuce, and anus. Other accompanied lesions may include enlarged submandibular lymph nodes and non-septic suppurative arthritis (which were not present in this case).
Often the skin lesions will form fistulas and drain, and the pustules will rupture and form ulcers and crusts. Secondary bacterial infections are common. The pathogenesis remains unknown but the dramatic response to immunosuppressive dosages of glucocorticoids supports the likelihood of an underlying immune dysfunction. Suppression of in vitro lymphocyte blastogenesis secondary to a serum factor has been documented in a few reports. It is also reported to have hereditary basis affecting mostly Dachshunds.
This condition could be diagnosed based on clinical presentation and age of the dog. However, initial presentation may resemble angioedema due to marked swelling of the face. At 24 to 48 hours after, the condition needs to be differentiated from severe generalized demodicosis, pyoderma secondary to immunodeficiency, and drug eruption.
It is recommended to complete a cytological examination, skin scrapings and swab collection to rule out demodicosis and primary bacterial infection. Histopathological examination of the skin biopsies is required for definitive diagnosis.
BIOPSY COLLECTION TECHNIQUE
It is often recommended to collect multiple punch biopsy specimens (4 or 6 mm in diameter) should be taken from intact pustules, vesicles, or nodules. A wedge biopsy or 8 mm punch biopsies are NOT RECOMMENDED as the skin becomes very friable in this condition and will be difficult to suture. It is impossible to definitively diagnose this condition without accompanied clinical history and age of the patient; histopathologically differentiating from sterile granuloma and pyogranuloma syndrome is impossible.
Note: References available upon request.
NEXT: Diagnostic Approach to Peritoneal Effusions
Return to Index