March 2021
Diagnosing Nutritional Issues in Beef Cattle: Part II
By Dr. Gregg Hanzlicek
The first article in this series (published in the January edition of Diagnostic Insights for Veterinarians ) discussed diagnosing energy and protein malnutrition in cow-calf herds. This article discusses the diagnosis of macro mineral deficiencies.
Calcium is stored in large quantities in bone and homeostasis is minutely regulated by parathyroid hormone (PTH).1 Typically, when calcium issues are observed in beef cows they are secondary to hypomagnesemia and not primary calcium issues.1 Simply, to maintain calcium homeostasis, PTH requires magnesium to effectively bind with renal and bone receptors.
Magnesium deficiency is the most common macromineral deficiency observed in beef-cows during the calving season.Magnesium homeostasis is unique; although there is large amount of Magnesium stored in bone and teeth, the cow does not have an efficient, functional way to access these stores. Her metabolic magnesium requirements are almost entirely dependent on adequate dietary magnesium consumption and absorption.
Even when adequate magnesium is consumed, there are several other factors that can reduce its availability.1 1) As bovines age, their ability to absorb dietary magnesium decreases. 2) Magnesium availability is decreased in diets that contain large amounts of forage due to elevated rumen pH. 3) Excessive dietary potassium can interfere with the active transport of magnesium through the rumen wall. 4) Active magnesium transport through the rumen wall is decreased in diets that contain insufficient dietary sodium. 5) The physical form of magnesium oxide (the most common source of magnesium in mineral packs) can reduce availability. Coarse magnesium oxides are poorly available to the cow in comparison to finely ground forms. One or more of the above-mentioned factors can be present in a herd simultaneously.
Antemortem diagnosis of deficiencies:
Antemortem subclinical hypomagnesemia diagnosis is accomplished by sampling 12-18 normal healthy adult cows (in any group that contains ≤300). If 20% or more of the serum samples contain <1.9 mg/dL magnesium, there is evidence that the herd is experiencing hypomagnesemia. The same samples can be used for subclinical calcium analysis. If 20% or more of the samples contain <8.0 mg/dL calcium, hypocalcemia is likely a herd issue.
Postmortem diagnosis of deficiencies:
Postmortem ocular tests should not be the sole diagnostic criteria, but more appropriately should be used in conjunction with other information including, clinical signs, history, diet, etc.
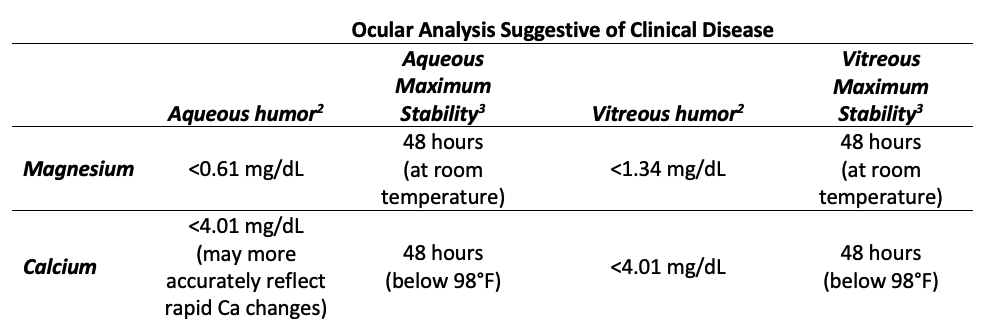

Ocular magnesium concentrations can significantly change 48 hours post death. Values may increase if cellular debris is present and decrease if bacterial contamination has occurred.2 One way to estimate the time-of-death is through ocular potassium analysis. Although there are no clear time of death guidelines for bovines, research suggests potassium levels increase approximately 2.5 mEq/L every 12 hours after death.4 Normal ocular fluid potassium concentration is approximately 30% lower than serum concentrations.5 Therefore, an ocular fluid concentration of ≥10.0 mEq/L would suggest the time of death was not within the previous 48 hours, and the assay magnesium levels may not reflect true magnesium or calcium status.
More information
KSVDL’s postmortem hypomagnesemia panel (CP-2216) includes both magnesium and potassium.
See our YouTube video on how to collect aqueous and vitreous humor, please follow this link: Sampling ocular fluids
References:
- Goff. Calcium and Magnesium Disorders. Veterinary Clinics of North America. 2014 (30) 359-381
- Edwards, Foster, Livesey. Use of Ocular Fluids to Aid Postmortem Diagnosis in Cattle and Sheep. In Practice. 2009 (31) 22-25
- McCoy, Hutchinson, Davison, et al. Postmortem Biochemical Markers of Experimentally Induced Hypomagnesemia Tetany in Cattle. The Veterinary Record. 2001 (148), 268-273
- Lincoln, Lane. Postmortem Chemical Analysis of Vitreous Humor as a Diagnostic Aid in Cattle. Modern Veterinary Practice: Food Animal. 1985 (65) 883-886
- Cornell University College of Veterinary Medicine: eClinpath. 2021 https://eclinpath.com/chemistry/ocular-fluids/